When Consent Changes on the Table
A patient story about spinal injections, medical trauma, and the long road to diagnosing a rare spinal condition.
Content note: This reflection discusses medical trauma and loss of control within healthcare experiences, which may be difficult for some readers.
About a year into trying to understand the pain in my spine after I was in a serious motor vehicle accident, I was seeing both a neurosurgeon and a pain management doctor. At that point I had already begun researching Tarlov cyst disease and cerebrospinal fluid leaks. I knew enough to understand that certain procedures commonly used for back pain can be risky for patients with fragile dura or perineural cysts.
Because of that, I had been clear from the beginning that I did not want injections into my spine.
The neurosurgeon in the office suggested something that sounded more reasonable. An SI joint injection on the right side. The purpose was simply diagnostic. If the sacroiliac joint responded to the injection, it might explain the pain. If it did not, we could continue investigating other causes before moving forward with more invasive testing like a myelogram.
That seemed fair.
So I drove myself to the appointment.
I remember signing the consent form quickly. I was nervous, but I believed we were doing the procedure we had discussed. I planned to go through it without sedation or pain medication, just breathing and getting through it.
When I walked into the procedure room, the music was blaring. Loud music filled with explicit lyrics. I was trying to calm myself and focus on breathing, but it was impossible to concentrate. Eventually I asked the nurse to turn it off.
Then the procedure began.
It was image guided. As the needle was placed, I felt something I had never felt before. A sharp electrical sensation shot down my leg. A sudden zing through the sciatic nerve that made my whole body tense.
Then my right leg became weak.
Not numb exactly. Just weak. As if the strength had drained out of it.
I had driven myself there, so I had to drive home. But I remember sitting in the parking lot for a long time first because my leg did not feel stable enough to leave right away.
Over the next several hours the pain began to escalate.
And it kept escalating.
Within days the pain had become so intense that I would go on the back deck at all times of the night, stare off into the woods in the back of our house in the middle of the night, screaming in my head from the pain, but crying quietly outside. I kept replaying the procedure in my mind and asking myself the same question.
What just happened? How could I feel this terrible after an SI joint injection?
When I contacted the office about the worsening pain, they told me to go to the emergency room. That something else must be wrong. That a procedure like this would not cause that much pain.
Sketchbook Reflection
I created this page during a time when I was trying to make sense of what my body was going through. The quote by Carl Jung stopped me when I first read it: “There is no coming to consciousness without pain.”
At the time, I did not yet have answers for what was happening in my spine. I only knew that something was wrong, and that becoming aware of it meant confronting a reality that others were not yet seeing.
Looking back now, this page feels like a quiet marker in the middle of that journey. Awareness can be painful, but it is also the beginning of understanding, and sometimes the beginning of reclaiming your voice. This sketch was drawn during this time.
When Pain Is Dismissed
The days after that injection were some of the most frightening of my medical journey. The pain was escalating rapidly, and I could feel that something in my body was not reacting normally.
Eventually I went to the emergency room, hoping someone would at least evaluate whether the injection had caused damage.
By that point I had discovered that the only position that brought temporary relief was squatting. It sounds strange, but it allowed a small release of pressure in my back. I could briefly reduce the pain that way.
The physician assistant who evaluated me focused on that moment.
Because I was able to squat down and lift my backpack, he questioned whether I could really be experiencing severe back pain. I tried to explain that the pain had dramatically worsened immediately after the injection and that something felt very wrong.
Instead of focusing on the new symptoms, the conversation shifted in another direction.
He told me he had “looked me up” and asked why I had been “upstairs” before. When he gestured toward the upper floors of the hospital and asked what he meant, he repeated himself slowly and gestured something strange with his hands and eyebrows. I realized he was implying psychiatric treatment that I had.
The problem was that I had never been admitted to that hospital.
The only time I had ever been in that building was as a nursing student completing clinical rotations during COVID.
In that moment it became clear that my concerns were being filtered through a different lens. Not a neurological one. A psychological one.
I had come seeking evaluation after a spinal procedure that had caused sudden and escalating pain. What I encountered instead was suspicion.
When I asked if imaging could be done to make sure nothing had gone wrong with my spine, the request was brushed aside. Instead, I was offered another injection.
After what had just happened to my body, I declined.
And then I walked out.
Later I reported the interaction through the hospital’s patient advocacy channels because the bias was so clear. I explained exactly what had happened and how my concerns had been dismissed. I was told it would be reviewed.
Nothing ever came of it.
There was no follow up. No explanation. No acknowledgement. I called three separate times. I wrote a letter. And still, there was never any follow up of any kind.
Looking back now, the pattern is painfully obvious.
First there was the physical violation of consent with the unexpected spinal injection.
Then there was the medical dismissal that followed, where escalating pain was interpreted through the lens of mental health history rather than investigated as a possible complication.
When patients carry psychiatric diagnoses in their charts, it can quietly change how their physical symptoms are interpreted. Even when those symptoms are new, sudden, and medically significant.
For me, that moment became one of the clearest examples of how easily real neurological suffering can be minimized when bias enters the room.
Ten days later I returned to the pain management office for a follow up.
The medical assistant looked at my chart and asked if I was there regarding my L4 L5 transforaminal steroid injection.
I told her no. I had come in for an SI joint injection.
She looked back at the chart again.
“No,” she said. “It says you had an L4 L5 transforaminal injection.”
When the physician came into the room, I asked him about it directly.
He confirmed that he had changed the procedure.
He said he did not believe the SI joint was the source of the pain, so he had performed the spinal injection instead.
I remember sitting there stunned.
That was the procedure I had specifically said I did not want.
At that point I did not yet have confirmation of the extent of the perineural cysts throughout my spine. I also did not yet know about the CSF venous fistula that would eventually be discovered at T7 and T8.
But I already knew that injections into the spine were something I had tried to avoid.
When I asked if the injection could have irritated a nerve root or a cyst, the concern was brushed aside.
“It’s not that big of a deal.”
But my body was telling a very different story.
I went home that day and sobbed to my husband.
“They injected my spine,” I told him. “I told them not to.”
That moment marked the beginning of a dramatic escalation in my neurological pain. Everything became worse. The sacral pain intensified. The nerve pain became more volatile. My sense of safety within medical procedures disappeared.
To make matters even more difficult, when I returned to the neurosurgeon who had originally suggested the SI joint test, he told me he could not move forward with treatment until an SI joint injection had been attempted.
The same injection I had originally agreed to.
But by that point I could not continue care within that system. I no longer trusted that the procedure discussed with me would be the procedure performed.
So I left and started over somewhere else.
Years later I now have confirmation of a CSF venous fistula and perineural cysts throughout my spine. I have undergone myelograms and continue navigating the long recovery from procedures that most people will never need to think about.
People sometimes wonder why patients with complex spinal conditions approach procedures with caution, fear, or hesitation.
This is why.
Sometimes the moment that changes everything begins with what was supposed to be a simple test.
When Consent Is Broken
There is another layer to experiences like this that is rarely discussed in medical spaces.
When a procedure is performed that a patient did not believe they had agreed to, the physical pain is only part of the impact. What lingers much longer is the psychological rupture that occurs when trust is broken in a vulnerable moment.
Medical procedures require surrender. A patient lies still while someone else approaches the most fragile parts of their body. They trust that the plan discussed beforehand is the plan that will be followed. That trust is not a small thing. It is the foundation that makes medical care possible.
When that boundary is crossed, something deeper than the body is affected.
For many patients, medical trauma does not begin in the hospital. It intersects with earlier experiences of powerlessness that shaped how safety and control were learned in the first place. When a person has already lived through moments in life where control was taken away from them, even subtle violations of consent in medical settings can reopen that psychological wound.
The body remembers what it feels like to lose control.
That moment in the procedure room did not just create pain in my spine. It created a feeling that the rules of safety had quietly changed without my knowledge. The plan had shifted while I was lying on the table, trusting that the conversation we had beforehand still mattered.
For someone who has spent years learning how to rebuild a sense of autonomy and personal boundaries, that experience can be deeply destabilizing.
Medical trauma is more common than most people realize. Research increasingly shows that patients who experience unexpected procedures, dismissive responses to pain, or violations of consent often carry long lasting psychological effects. Anxiety around future care. Hypervigilance during procedures. Difficulty trusting physicians even when they are trying to help.
What happened that day changed how I approach medicine.
But it also forced something important to grow.
For most of my life I tried to be the cooperative patient. The agreeable one. The person who trusted that the professionals knew best and that my role was simply to endure whatever was necessary to find answers.
That approach no longer works for me.
Living through experiences like this has required me to develop something stronger than cooperation. It has required boundaries.
Clear questions. Written documentation. Slower consent. The willingness to stop care when trust is broken. The courage to leave institutions where my voice is not respected.
Those boundaries were not something I naturally carried before this journey. They are something that had to be built through painful experience.
And in time, the medical picture around my spine became clearer.
Years later imaging would confirm what my body had been trying to communicate all along. A cerebrospinal fluid venous fistula in my thoracic spine. Perineural cysts throughout my spine. Fragile nerve root structures that can react intensely to procedures that are routine for most patients.
Knowing that now reframes that moment in the procedure room.
The concerns I had about spinal injections were not irrational fears. They were early instincts about a structural problem that had not yet been fully discovered.
Ironically, the same experience that created one of the most violating chapters of my medical journey also became a turning point in how I advocate for myself.
I still believe deeply in medicine. I have met extraordinary physicians who listen, who collaborate, and who treat patients as partners in the process of healing.
But trust must be mutual.
Consent must be real.
And when patients say that certain procedures feel unsafe for their bodies, that concern deserves to be taken seriously.
Especially when the patient has already lived through enough moments of powerlessness to know exactly what that feeling means.
Sketchbook Reflection
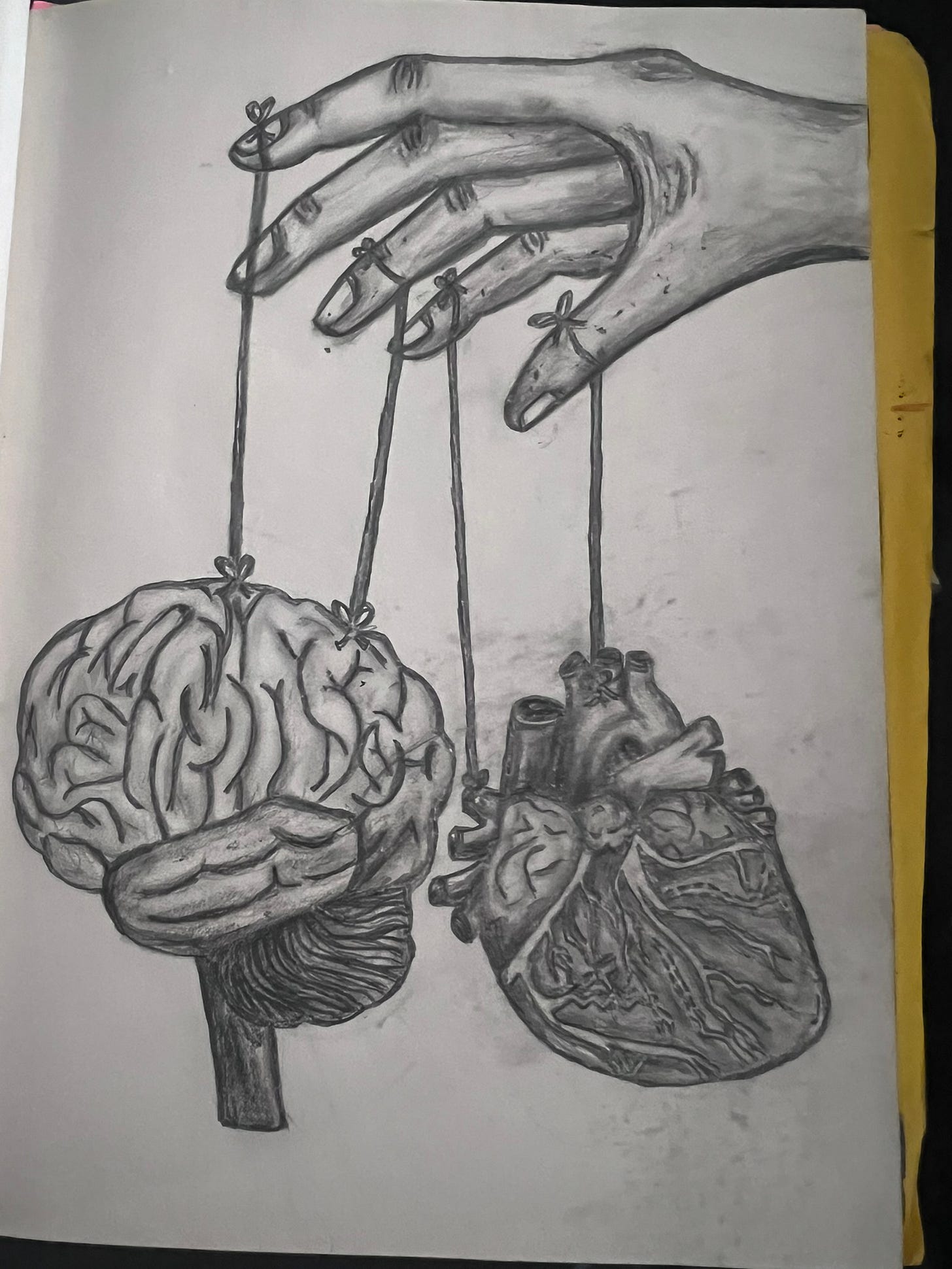
This drawing was inspired by an image I originally saw on Pinterest. The concept is not my own, but the interpretation and meaning behind it became personal as I sketched it. It lives in my sketchbook among many quiet drawings from a time when I was trying to understand what was happening inside my body.
During that period of my medical journey, my mind and heart often felt like they were being pulled in different directions. I was searching for answers while also trying to emotionally survive the uncertainty, the pain, and the medical experiences that often left me feeling powerless. Drawing became one way to process those feelings.
At the time I created this sketch, I did not yet have confirmation of the structural problems in my spine that would eventually be discovered. Later imaging would reveal a cerebrospinal fluid venous fistula and perineural cysts throughout my spine, helping explain why my brain, body, and emotions had felt so unsettled for so long.
Looking back at this piece now, I see it as a snapshot of that moment in time. A reminder of how deeply the experience of illness can affect both the brain that tries to make sense of it and the heart that carries its emotional weight.
Over time, my understanding shifted. What once felt like invisible strings of control began to look more like the quiet presence of something steady guiding me through the chaos. I titled it, “God is the Ultimate Puppeteer.”
Moving Forward
Even now, I am still processing the psychological impact of those experiences.
Medical trauma does not disappear the moment a diagnosis is finally found. The body remembers what it felt like to be dismissed, misunderstood, or treated as though its pain was imaginary. When those experiences intersect with mental health history, the effect can be even more destabilizing. The very support systems meant to help a person heal can sometimes become the lens through which their physical suffering is minimized.
In the years since these events, I have often revisited the evidence I kept during that time. Videos recorded in the middle of the night when the pain was escalating. Photos documenting changes in my body that I did not yet have words for. Notes, timelines, and medical records that helped me track what was happening when no one else seemed to see the pattern.
At the time, those recordings were simply acts of survival. I needed proof that what I was experiencing was real.
Looking back now, they have become something else. Documentation. A record of a body trying to communicate what medicine had not yet understood.
Those files tell the story of a patient navigating pain, fear, and uncertainty while trying to advocate for herself in systems that were not always prepared to listen.
And this story is only one chapter.
It represents just a few moments within a three-year journey of searching for answers, enduring procedures, confronting bias, and slowly learning how to rebuild trust in my own voice.
My hope in sharing it is not to assign blame. It is to invite reflection.
Patients with complex or rare conditions often arrive in medical spaces carrying layers of history. Physical pain. Emotional exhaustion. Sometimes psychiatric care that was meant to support them but instead becomes a label that shapes how their bodies are interpreted.
What we need from medicine is not perfection. We need curiosity. Careful listening. And a willingness to investigate when a patient says something has changed in their body.
Because sometimes the story a patient is telling is not a psychological one.
Sometimes it is a neurological one that simply has not been discovered yet.
And sometimes the difference between dismissal and discovery begins with the decision to take that story seriously.
Where Things Stand Now
Today, the picture of my spine looks very different than it did during those early years when I was searching for answers.
Imaging has now confirmed that I have diffuse perineural cysts throughout my spine, along with dural ectasia affecting the sacral region of the spinal cord. I underwent Tarlov cyst surgery to address cysts at S2, S3, S4, and S5, and during that procedure the sacral dural ectasia was also treated as part of the repair.
There is also a longstanding injury in my cervical spine that continues to be evaluated.
More recently, physicians identified a cerebrospinal fluid venous fistula, a rare type of spinal CSF leak that can cause profound neurological symptoms when spinal fluid drains where it should not. That discovery has helped explain many of the symptoms that once seemed disconnected and mysterious.
For the first time in this journey, the pieces of the puzzle are beginning to align.
I now have an upcoming procedure intended to seal that leak. My hope is simple. If the procedure is successful, it may allow my brain and spine to stabilize enough that I can remain upright longer, regain some strength, and slowly return to the creative work and advocacy that have carried me through this experience.
I do not expect everything to return to the way it was before. But I do hope for more time in the world outside of bed. More time with my family. More time creating. More time helping others navigate the kinds of medical systems that so many patients struggle to be heard within.
Because if this journey has taught me anything, it is that stories like mine are not rare.
And the future of patient care will depend on how willing we are to listen to them.
I am hopeful that this next procedure will allow my body a little more stability and a little more time upright in the world. Enough time to create, to advocate, and to help make sure that patients who come after me are listened to sooner than I was.
A Kinder Rewrite for the Doctors Who Care for Patients Like Me
I know that medicine is not easy.
Emergency rooms are busy. Pain is difficult to measure. And when a patient arrives with complex symptoms, incomplete answers, and a long history of medical notes, it can be hard to know where to begin.
I also understand that mental health histories appear in charts for good reasons. Many patients need that care and deserve it.
But I hope my story offers a gentle reminder of something important.
When a patient says that something has suddenly changed in their body, especially after a procedure, that moment deserves curiosity.
Not every unusual symptom is psychological.
Not every anxious patient is exaggerating.
And not every complex story is a sign of instability.
Sometimes it is simply a person whose body is trying to explain something that medicine has not yet discovered.
In my case, years later, imaging would show diffuse perineural cysts throughout my spine, sacral disease that required surgery, dural ectasia that had to be repaired, and a cerebrospinal fluid venous fistula that had been quietly altering my neurological function.
The story my body was telling was real. It just took time for the evidence to catch up.
Patients do not expect physicians to have every answer immediately. What we hope for is something simpler.
Careful listening.
Clear communication and documentation.
And the reassurance that when we say something feels wrong, that concern will be taken seriously.
Those small moments of curiosity can change the entire trajectory of a patient’s journey.
Because sometimes the difference between dismissal and discovery begins with a doctor who pauses long enough to ask one more question.
If sharing this story helps even one patient be heard a little sooner, or one physician pause long enough to listen more closely, then the pain that shaped it will not have been carried in vain.





I'm so sorry this happened to you. It's an outrage. What is wrong with our system that such incompetent doctors are able to continue practicing? He ought to be prosecuted for aggravated assault.
Thank you for speaking out about your experience.